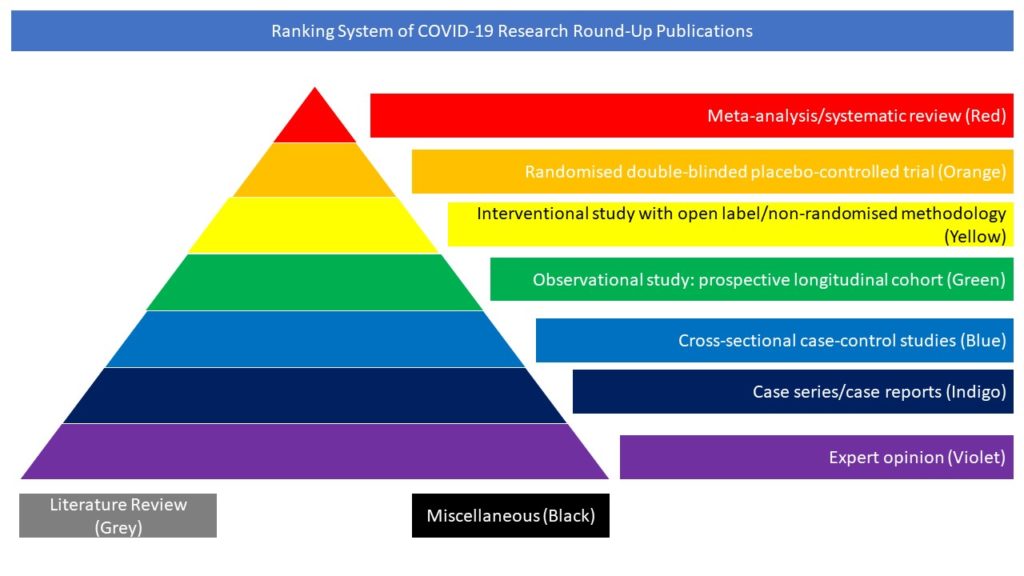
Cross-sectional case-control studies (Blue)
Read on for our pick of COVID-19-related cross-sectional case control studies from the scientific press for December 2022:
- Morbidity and severity of COVID-19 in patients with Parkinson’s disease treated with amantadine – A multicenter, retrospective, observational study
- The decline in stroke hospitalization due to COVID-19 is unrelated to COVID-19 intensity
Morbidity and severity of COVID-19 in patients with Parkinson’s disease treated with amantadine – A multicenter, retrospective, observational study
After more than 2 years of the pandemic, effective treatment for COVID-19 is still under research. In recent months, publications hypothesized amantadine’s potential beneficial effect on SARS-CoV-2 infection. The objective of this observational, retrospective, multicenter cohort study was to compare the groups of Parkinson’s Disease (PD) patients who were administered amantadine chronically and those who did not take this medication in the context of the incidence and severity of COVID-19 infection. The structured questionnaires were completed during the patient’s follow-up visits at the Outpatient Clinic or during hospitalization. The questionnaire included the following information: patient’s age, duration of PD, Hoehn-Yahr (H-Y) stage, comorbidities, medications, COVID-19 confirmed by reverse transcription polymerase chain reaction (RT-PCR) swab test for SARS-CoV-2 with specified symptoms and their severity (home or hospital treatment). The vaccination status was verified as well. Five hundred fifty-two (n = 552) patients participated in the study – 329 men (60%). The mean H-Y stage was 2.44 (range: 1-4) and the mean duration of PD was 9.6 years (range: 1-34). One hundred four subjects (19%) had confirmed COVID-19 infection. Subjects over 50 years of age had a significantly lower incidence of COVID-19 (17% vs 38%, p = 0.0001) with difference also in mean H-Y stage (2.27 vs 2.49; p = 0.011) and disease duration (8.4 vs 9.9 years, p = 0.007). There were no differences between patients with and without co-morbidities. In the whole analyzed group 219 (40%) subjects were treated with amantadine. Comparing COVID-19 positive and negative patients, amantadine was used by 48/104 (46%) and 171/448 (38%) respectively. 22% of patients on amantadine vs. 17% of patients without amantadine developed COVID-19. These differences were not significant. There were no differences in morbidity and severity of COVID-19 between amantadine users and non-users as well. The authors concluded that COVID-19 was less common in older (>50) with longer duration and more advanced patients. Amantadine did not affect the risk of developing COVID-19 or the severity of infection.
Przytuła F, Kasprzak J, Dulski J, Koziorowski D, Kwaśniak-Butowska M, Sołtan W, Roszmann A, Śmiłowska K, Schinwelski M, Sławek J. Morbidity and severity of COVID-19 in patients with Parkinson’s disease treated with amantadine – A multicenter, retrospective, observational study. Parkinsonism Relat Disord. 2022 Dec 6;106:105238. doi: 10.1016/j.parkreldis.2022.105238.
The decline in stroke hospitalization due to COVID-19 is unrelated to COVID-19 intensity
During the COVID-19 pandemic many countries reported a decline in stroke volumes. The aim of this study was to analyze if the decline was related to intensity of the COVID-19 pandemic.
The authors compared the first pandemic year (March 1, 2020, to February 28, 2021) overall and during the three COVID-19 waves with the preceding year. Volumes of acute ischemic stroke (AIS), subarachnoid hemorrhage (SAH), intracerebral hemorrhage (ICH), and recanalization treatments [intravenous thrombolysis (IVT) and mechanical thrombectomy (MT)] were obtained from the National Register of Reimbursed Health Services. Door-to-needle time (DNT), onset-to-door time (ODT), and NIHSS at admission were obtained from RES-Q. During the pandemic year as compared to the preceding year there were 26,453 vs 28,771 stroke admissions, representing an 8.8% decline (p<0.001). The decline (-10%, -11%, -19%) appeared in all COVID-19 waves (spring 2020, autumn 2020, winter 2021), except for an increase (2%) during summer 2020. Admissions for AIS declined by 10.2%, p<0.001), while hemorrhagic stroke volumes were minimally decreased. The absolute volumes of IVT and MT decreased by 9.4% (p<0.001) and 5.7% (p=0.16), respectively. However, the proportions of ischemic stroke patients receiving IVT (18% vs 18%; p=0.72) and MT (6% vs 6%; p=0.28) remained unchanged. The authors concluded that there was a decline in stroke admissions, but such decline was not related to COVID-19 incidence. The frequency of use of recanalization procedures (IVT, MT) and times (ODT, DNT) in AIS were preserved in the Czech Republic during the first year of the pandemic.
Sedova P, Kent JA, Bryndziar T, Jarkovsky J, Tomek A, Sramek M, Skoda O, Sramkova T, Pokorová K, Littnerova S, Brown RD Jr, Mikulik R. The decline in stroke hospitalization due to COVID-19 is unrelated to COVID-19 intensity. Eur J Neurol. 2022 Dec 13. doi: 10.1111/ene.15664.