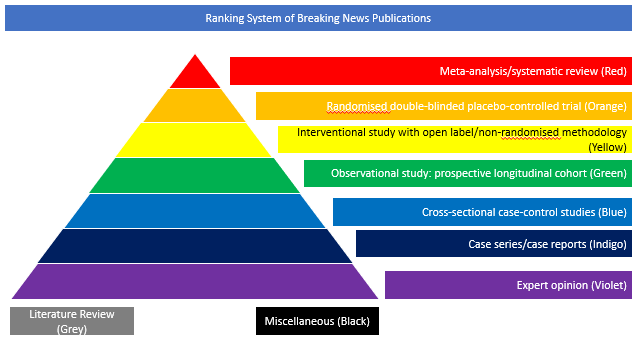
Meta-analysis/Systematic Review (Red)
In this paper the authors conducted a systematic review on cerebrovascular events in COVID-19 infection. A comprehensive literature search was performed including articles published from January 1, 2020, to July 23, 2020. Additional sources were added by the authors by reviewing related references. The systematic review was conducted in accordance with the PRISMA guidelines. Only articles reporting individual data on stroke mechanism and aetiology, sex, age, past cardiovascular risk factors, COVID symptoms, admission stroke severity score (NIHSS), D-dimer levels, and acute stroke treatment were selected for the review. Articles that did not report the clinical description of the cases were excluded. A descriptive statistical analysis of the data collected was performed. From a total of 1,210 articles published from January 1, 2020, to July 23, 2020, 80 articles (275 patients), which satisfied the abovementioned criteria, were included in this review. A total of 226 cases of ischaemic stroke (IS), 35 cases of intracranial bleeding, and 14 cases of cerebral venous sinus thrombosis (CVST) were found. Among patients with IS, the mean age was 64.16 ±14.73 years (range 27–92 years) and 53.5% were male. The mean NIHSS score reported at the onset of stroke was 15.23 ±9.72 (range 0–40). Primary endovascular thrombectomy (EVT) was performed in 24/168 patients (14.29%), intravenous thrombolysis (IVT) was performed in 17/168 patients (10.12%), and combined IVT+EVT was performed in 11/168 patients (6.55%). According to the reported presence of large vessel occlusion (LVO) (105 patients), 31 patients (29.52%) underwent primary EVT or bridging. Acute intracranial bleeding was reported in 35 patients: 24 patients (68.57%) had intracerebral haemorrhage (ICH), 4 patients (11.43%) had non-traumatic subarachnoid haemorrhage (SAH), and the remaining 7 patients (20%) had the simultaneous presence of SAH and ICH. Fourteen cases of CVST were reported in the literature (50% males), mean age 42.8 years ±15.47 (range 23–72). Treatment was reported only in nine patients; seven were treated with anticoagulant therapy; one with acetazolamide, and one underwent venous mechanical thrombectomy.
The authors concluded that cerebrovascular events are relatively common findings in COVID-19 infection, and they could have a multifactorial etiology. More accurate and prospective data are needed to better understand the impact of cerebrovascular events in COVID-19 infection.
DOI: https://doi.org/10.3389/fneur.2020.574694