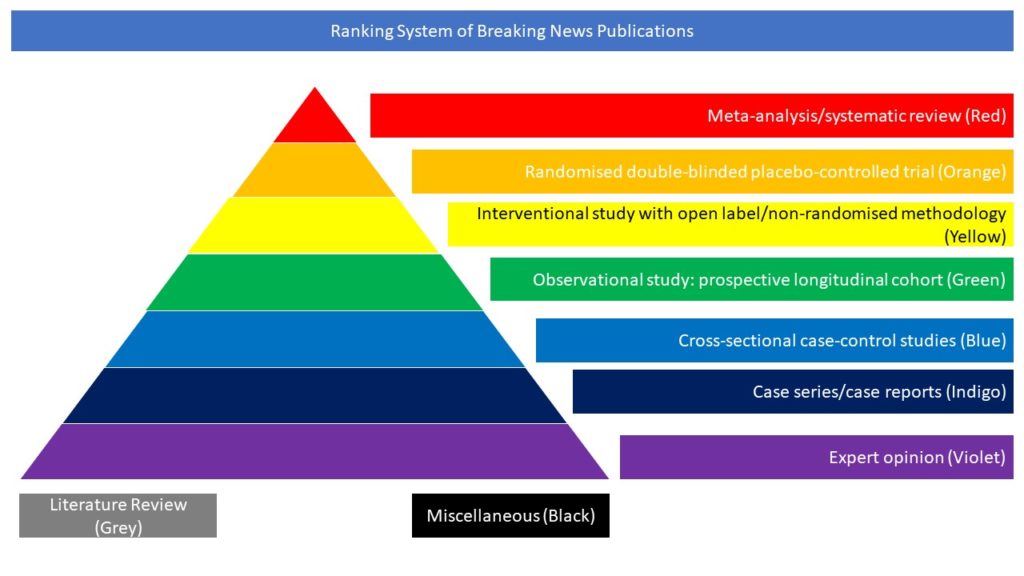
Miscellaneous (Black)
Read on for our highlighted selection of miscellaneous Covid-related studies from the scientific press for January 2022
- Omicron escapes the majority of existing SARS-CoV-2 neutralizing antibodies
- Evolution of enhanced innate immune evasion by SARS-CoV-2
- SARS-CoV-2 Omicron variant shows less efficient replication and fusion activity when compared with delta variant in TMPRSS2-expressed cells
Omicron escapes the majority of existing SARS-CoV-2 neutralizing antibodies
The SARS-CoV-2 B.1.1.529 variant (Omicron) contains 15 mutations on the receptor-binding domain (RBD). How Omicron would evade RBD neutralizing antibodies (NAbs) requires immediate investigation. In this article the authors used high-throughput yeast display screening to determine the RBD escaping mutation profiles for 247 human anti-RBD NAbs and showed that the NAbs could be unsupervised clustered into six epitope groups (A-F), which is highly concordant with knowledge-based structural classifications. Strikingly, various single mutations of Omicron could impair Nabs of different epitope groups. Specifically, NAbs in Group A-D, whose epitope overlap with ACE2-binding motif, are largely escaped by K417N, G446S, E484A, and Q493R. Group E (S309 site) and F (CR3022 site) NAbs, which often exhibit broad sarbecovirus neutralizing activity, are less affected by Omicron, but still, a subset of NAbs are escaped by G339D, N440K, and S371L. Furthermore, Omicron pseudovirus neutralization showed that single mutation tolerating NAbs could also be escaped due to multiple synergetic mutations on their epitopes. In total, over 85% of the tested Nabs are escaped by Omicron. Regarding NAb drugs, the neutralization potency of LY-CoV016/LY-CoV555, REGN10933/REGN10987, AZD1061/AZD8895, and BRII-196 were greatly reduced by Omicron, while VIR-7831 and DXP-604 still function at reduced efficacy. Together, these data suggest Omicron would cause significant humoral immune evasion, while NAbs targeting the sarbecovirus conserved region remain most effective. The authors concluded that their results offer instructions for developing NAb drugs and vaccines against Omicron and future variants.
Yunlong Cao , Jing Wang , Fanchong Jian , Tianhe Xiao , Weiliang Song , Ayijiang Yisimayi , Weijin Huang , Qianqian Li , Peng Wang , Ran An , Jing Wang , Yao Wang , Xiao Niu , Sijie Yang , Hui Liang , Haiyan Sun , Tao Li , Yuanling Yu , Qianqian Cui , Shuo Liu , Xiaodong Yang , Shuo Du , Zhiying Zhang , Xiaohua Hao , Fei Shao , Ronghua Jin , Xiangxi Wang , Junyu Xiao , Youchun Wang & Xiaoliang Sunney Xie. Omicron escapes the majority of existing SARS-CoV-2 neutralizing antibodies. Nature. doi: https://doi.org/10.1038/d41586-021-03796-6.
Evolution of enhanced innate immune evasion by SARS-CoV-2
Emergence of SARS-CoV-2 variants of concern (VOCs) suggests viral adaptation to enhance human-to-human transmission. Although much effort has focused on characterisation of spike changes in VOCs, mutations outside spike likely contribute to adaptation. In this article the authors used unbiased abundance proteomics, phosphoproteomics, RNAseq and viral replication assays to show that isolates of the Alpha (B.1.1.7) variant more effectively suppress innate immune responses in airway epithelial cells, compared to first wave isolates. They found that Alpha has dramatically increased subgenomic RNA and protein levels of N, Orf9b and Orf6, all known innate immune antagonists. Expression of Orf9b alone suppressed the innate immune response through interaction with TOM70, a mitochondrial protein required for RNA sensing adaptor MAVS activation. Moreover, the activity of Orf9b and its association with TOM70 was regulated by phosphorylation. The authors propose that more effective innate immune suppression, through enhanced expression of specific viral antagonist proteins, increases the likelihood of successful Alpha transmission, and may increase in vivo replication and duration of infection. The importance of mutations outside Spike in adaptation of SARS-CoV-2 to humans is underscored by the observation that similar mutations exist in the Delta and Omicron N/Orf9b regulatory regions.
Thorne, L.G., Bouhaddou, M., Reuschl, AK. et al. Evolution of enhanced innate immune evasion by SARS-CoV-2. Nature (2021). https://doi.org/10.1038/s41586-021-04352-y.
SARS-CoV-2 Omicron variant shows less efficient replication and fusion activity when compared with delta variant in TMPRSS2-expressed cells
The novel SARS-CoV-2 Omicron variant (B.1.1.529), first found in early November 2021, has sparked considerable global concern and it has >50 mutations, many of which are known to affect transmissibility or cause immune escape. In this study, the authors sought to investigate the virological characteristics of Omicron variant and compared it with the Delta variant which has dominated the world since mid-2021. Omicron variant replicated more slowly than the Delta variant in transmembrane serine protease 2 (TMPRSS2)-overexpressing VeroE6 (VeroE6/TMPRSS2) cells. Notably, the Delta variant replicated well in Calu-3 cells which has robust TMPRSS2 expression, while the Omicron variant replicated poorly in this cell line. To confirm the difference in entry pathway between the Omicron and Delta variants, the authors assessed the antiviral effect of bafilomycin A1, chloroquine (inhibiting endocytic pathway) and camostat (inhibiting TMPRSS2 pathway). Camostat potently inhibit the Delta variant but not the Omicron variant, while bafilomycin A1 and chloroquine could inhibit both Omicron and Delta variants. Moreover, Omicron variant also showed weaker cell-cell fusion activity when compared with Delta variant in VeroE6/TMPRSS2 cells. Collectively, their results suggest that Omicron variant infection is not enhanced by TMPRSS2 but is largely mediated via the endocytic pathway. The difference in entry pathway between Omicron and Delta variant may have implication on the clinical manifestations or disease severity.
Zhao H, Lu L, Peng Z, Chen LL, Meng X, Zhang C, Ip JD, Chan WM, Chu AW, Chan KH, Jin DY, Chen H, Yuen KY, To KK. SARS-CoV-2 Omicron variant shows less efficient replication and fusion activity when compared with delta variant in TMPRSS2-expressed cells. Emerg Microbes Infect. 2021 Dec 24:1-18. doi: 10.1080/22221751.2021.2023329.