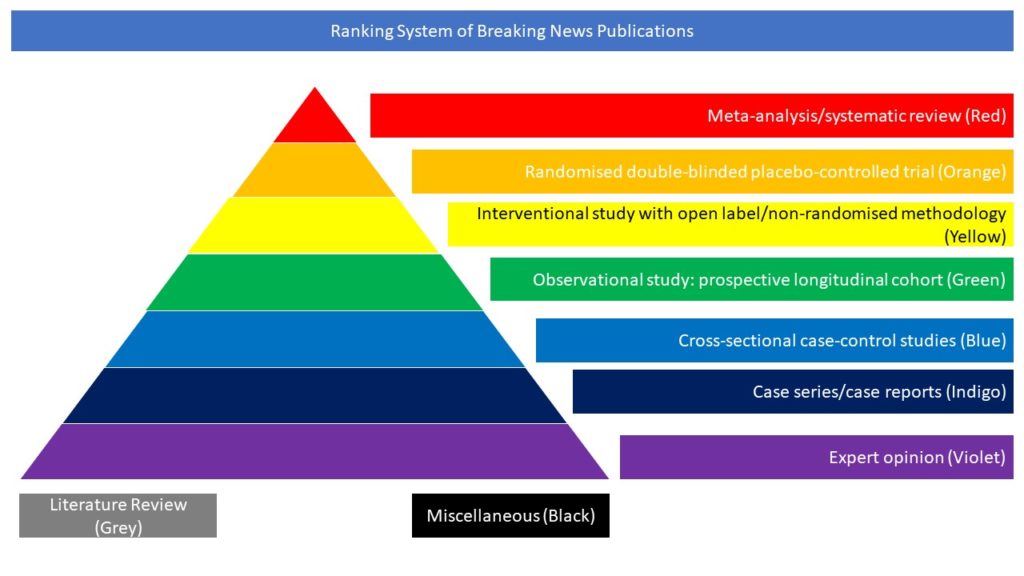
Cross-sectional case-control studies (Blue)
Read on for our highlighted selection of Covid-related cross-sectional case control studies from the scientific press for February 2022:
- Association of Major Depressive Symptoms With Endorsement of COVID-19 Vaccine Misinformation Among US Adults
- Comparison of serum neurodegenerative biomarkers among hospitalized COVID-19 patients versus non-COVID subjects with normal cognition, mild cognitive impairment, or Alzheimer’s dementia
Association of Major Depressive Symptoms With Endorsement of COVID-19 Vaccine Misinformation Among US Adults
Misinformation about COVID-19 vaccination may contribute substantially to vaccine hesitancy and resistance. The objective of this study was to determine if depressive symptoms are associated with greater likelihood of believing vaccine-related misinformation. This survey study analyzed responses from 2 waves of a 50-state nonprobability internet survey conducted between May and July 2021, in which depressive symptoms were measured using the Patient Health Questionnaire 9-item (PHQ-9). Survey respondents were aged 18 and older. Population-reweighted multiple logistic regression was used to examine the association between moderate or greater depressive symptoms and endorsement of at least 1 item of vaccine misinformation, adjusted for sociodemographic features. The association between depressive symptoms in May and June, and new support for misinformation in the following wave was also examined. The main outcome was endorsing any of 4 common vaccine-related statements of misinformation. Among 15 464 survey respondents (9834 [63.6%] women and 5630 [36.4%] men; 722 Asian respondents [4.7%], 1494 Black respondents [9.7%], 1015 Hispanic respondents [6.6%], and 11 863 White respondents [76.7%]; mean [SD] age, 47.9 [17.5] years), 4164 respondents (26.9%) identified moderate or greater depressive symptoms on the PHQ-9, and 2964 respondents (19.2%) endorsed at least 1 vaccine-related statement of misinformation. Presence of depression was associated with increased likelihood of endorsing misinformation (crude odds ratio [OR], 2.33; 95% CI, 2.09-2.61; adjusted OR, 2.15; 95% CI, 1.91-2.43). Respondents endorsing at least 1 misinformation item were significantly less likely to be vaccinated (crude OR, 0.40; 95% CI, 0.36-0.45; adjusted OR, 0.45; 95% CI, 0.40-0.51) and more likely to report vaccine resistance (crude OR, 2.54; 95% CI, 2.21-2.91; adjusted OR, 2.68; 95% CI, 2.89-3.13). Among 2809 respondents who answered a subsequent survey in July, presence of depression in the first survey was associated with greater likelihood of endorsing more misinformation compared with the prior survey (crude OR, 1.98; 95% CI, 1.42-2.75; adjusted OR, 1.63; 95% CI, 1.14-2.33). The authors concluded that this survey study found that individuals with moderate or greater depressive symptoms were more likely to endorse vaccine-related misinformation, cross-sectionally and at a subsequent survey wave. While this study design cannot address causation, the association between depression and spread and impact of misinformation merits further investigation.
Perlis RH, Ognyanova K, Santillana M, Lin J, Druckman J, Lazer D, Green J, Simonson M, Baum MA, Della Volpe J. Association of Major Depressive Symptoms With Endorsement of COVID-19 Vaccine Misinformation Among US Adults. JAMA Netw Open. 2022 Jan 4;5(1):e2145697. doi: 10.1001/jamanetworkopen.2021.45697
Comparison of serum neurodegenerative biomarkers among hospitalized COVID-19 patients versus non-COVID subjects with normal cognition, mild cognitive impairment, or Alzheimer’s dementia
The authors measured the levels of several neurodegenerative markers in the serum, as total tau (t-tau), phosphorylated tau-181 (p-tau181), glial fibrillary acidic protein (GFAP), neurofilament light chain (NfL), ubiquitin carboxyterminal hydrolase L1 (UCHL1), amyloid Aβ (Aβ40,42), Aβ42/40 and p-tau181/Aβ42 ratios and inflammatory biomarkers as interleukin-6, C-reactive protein, D-dimer, and Ferritin in 251 COVID-19 patients without a prior dementia diagnosis. They compared patients with or without encephalopathy, in-hospital death versus survival, discharge home versus other outcomes and all COVID-19 patients versus healthy controls (54), Mild Cognitive Impairment (MCI) (54) and Alzheimer’s disease (AD) (53) patients. T-tau, p-tau181, GFAP, and NfL were significantly elevated in patients with encephalopathy and in those who died in-hospital, while t-tau, GFAP, and NfL were significantly lower in those discharged home. All neurodegenerative markers correlated with age, severity of COVID-19 illness (i.e. requiring mechanical ventilation, Sequential Organ Failure Assessment Score, lower oxygen saturations and mean arterial blood pressure), with T-tau, p-tau181 and NfL correlating more strongly with severity of illness. P-tau181, NfL and GFAP were also correlated with D-dimer levels. NfL and GFAP were higher in COVID patients than in controls, MCI or AD, and UCHL1 was higher in COVID-19 patients compared to controls and MCI patients.
Frontera JA, Boutajangout A, Masurkar AV, Betensky RA, Ge Y, Vedvyas A, Debure L, Moreira A, Lewis A, Huang J, Thawani S, Balcer L, Galetta S, Wisniewski T. Comparison of serum neurodegenerative biomarkers among hospitalized COVID-19 patients versus non-COVID subjects with normal cognition, mild cognitive impairment, or Alzheimer’s dementia. Alzheimers Dement. 2022 Jan 13. doi: 10.1002/alz.12556.