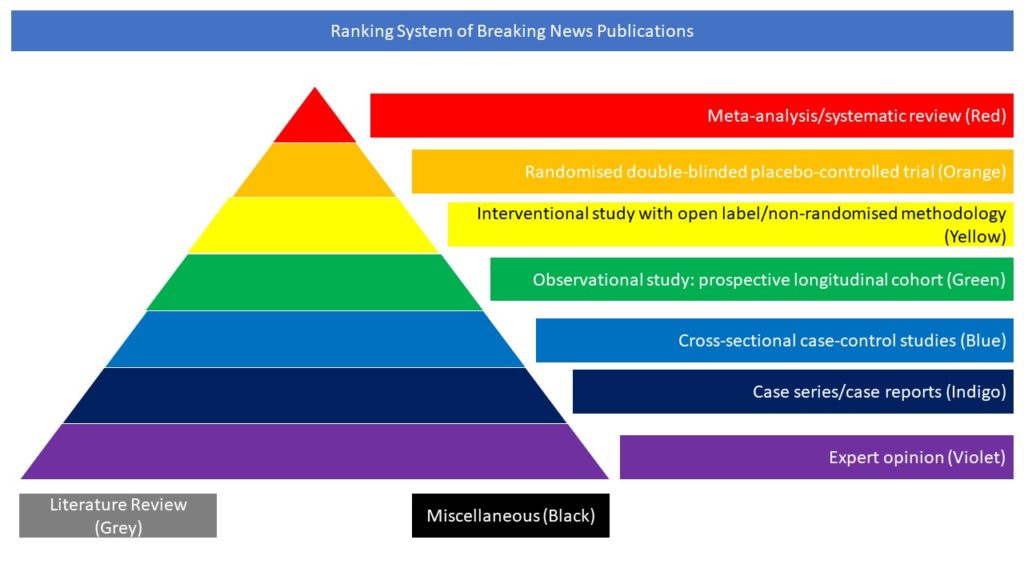
Case series/case reports (Indigo)
Stroke may complicate COVID-19 infection based on clinical hypercoagulability. In this article the authors investigated whether transcranial Doppler ultrasound has utility for identifying microemboli and clinically relevant cerebral blood flow velocities (CBFVs) in COVID-19. They performed transcranial Doppler for a consecutive series of patients with confirmed or suspected COVID-19 infection admitted to 2 intensive care units at a large academic center including evaluation for microembolic signals. Variables specific to hypercoagulability and blood flow including transthoracic echocardiography were analyzed as a part of routine care. Twenty-six patients were included in this analysis, 16 with confirmed COVID-19 infection. Of those, 2 had acute ischemic stroke secondary to large vessel occlusion. Ten non-COVID stroke patients were included for comparison. Two COVID-negative patients had severe acute respiratory distress syndrome and stroke due to large vessel occlusion. In patients with COVID-19, relatively low CBFVs were observed diffusely at median hospital day 4 (interquartile range, 3-9) despite low hematocrit (29.5% [25.7%-31.6%]); CBFVs in comparable COVID-negative stroke patients were significantly higher compared with COVID-positive stroke patients. Microembolic signals were not detected in any patient. Median left ventricular ejection fraction was 60% (interquartile range, 60%-65%). CBFVs were correlated with arterial oxygen content, and C-reactive protein (Spearman ρ=0.28 [P=0.04]; 0.58 [P<0.001], respectively) but not with left ventricular ejection fraction (ρ=-0.18; P=0.42). The authors concluded that in this cohort of critically ill patients with COVID-19 infection, they observed lower than expected CBFVs in setting of low arterial oxygen content and low hematocrit but not associated with suppression of cardiac output.
Ziai WC, Cho SM, Johansen MC, Ergin B, Bahouth MN. Transcranial Doppler in Acute COVID-19 Infection: Unexpected Associations. Stroke. 2021 Apr 21:STROKEAHA120032150. doi: 10.1161/STROKEAHA.120.032150. Epub ahead of print. PMID: 33878893