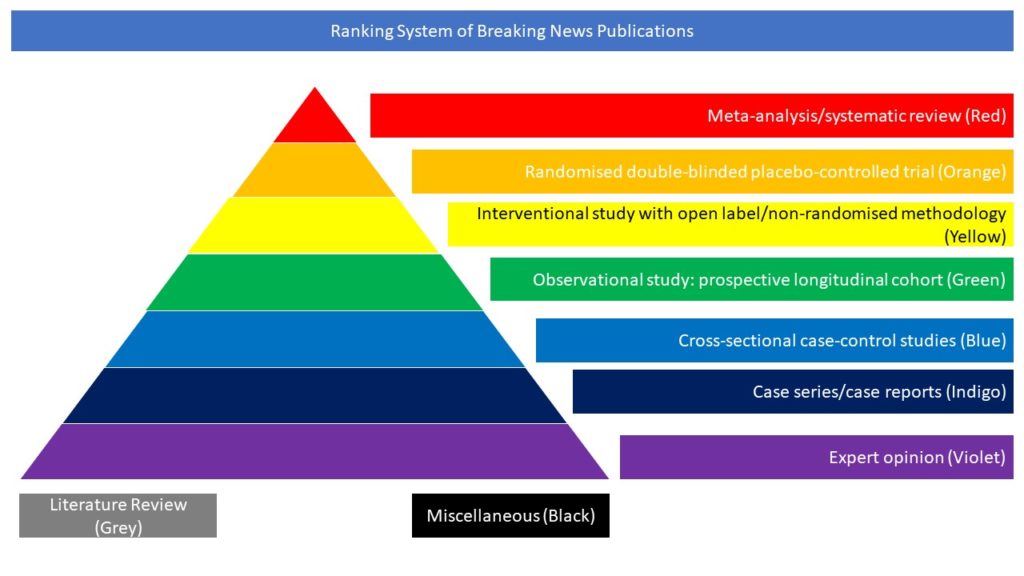
Cross-sectional case-control studies (Blue)
Read on for the second half of our highlighted selection of Covid-related cross-sectional case control studies from the scientific press for January 2022:
- Age-Stratified Risk of Cerebral Venous Sinus Thrombosis After SARS-CoV-2 Vaccination
- The Impact of the COVID-19 Pandemic on Creutzfeldt-Jakob Disease Surveillance and Patient Care in the United Kingdom
- Association of the COVID-19 Outbreak with Acute Stroke Care in Switzerland
- Multisystem Involvement in Post-acute Sequelae of COVID-19 (PASC)
- A longitudinal seizure outcome following the COVID-19 pandemic in 2020 and 2021: Transient exacerbation or sustainable mitigation
- APOE ε4 associates with increased risk of severe COVID-19, cerebral microhaemorrhages and post-COVID mental fatigue: a Finnish biobank, autopsy and clinical study
- Characteristics and Risk Factors of Persistent Neuropathic Pain in Recovered COVID-19 Patients
- Barriers to telemedicine among physicians in epilepsy care during the COVID-19 pandemic: A national-level cross-sectional survey in Japan
- Persistent white matter changes in recovered COVID-19 patients at the 1-year follow-up
- CD19 B cell repopulation after ocrelizumab, alemtuzumab and cladribine: Implications for SARS-CoV-2 vaccinations in multiple sclerosis
- Neurologic and cognitive sequelae after SARS-CoV2 infection: Different impairment for ICU patients
- Epilepsy is overrepresented among young people who died from COVID-19: Analysis of nationwide mortality data in Hungary
Age-Stratified Risk of Cerebral Venous Sinus Thrombosis After SARS-CoV-2 Vaccination
Cerebral Venous Sinus Thrombosis (CVST) as a part of the thrombosis and thrombocytopenia syndrome is a rare adverse drug reaction of SARS-CoV-2 vaccination. Estimated background rate of CVST with thrombocytopenia is 0.1 per million per month. In this article the authors assessed the age-stratified risk of CVST with and without thrombocytopenia after SARS- CoV-2 vaccination. They estimated the absolute risk of CVST with and without thrombocytopenia within 28 days of first dose of four SARS-CoV-2 vaccinations, using data from the European Medicines Agency’s EudraVigilance database (until 13 June 2021). As a denominator, they used data on vaccine delivery from 31 European countries. For 22.8 million adults from 25 countries, they estimated the absolute risk of CVST after the first dose of ChAdOx1 nCov-19 per age category. The absolute risk of CVST within 28 days of first dose vaccination was 7.5 (95%CI 6.9-8.3), 0.7 (95%CI 0.2-2.4), 0.6 (95%CI 0.5-0.7) and 0.6 (95%CI 0.3-1.1) per million of first doses of ChAdOx1 nCov-19, Ad26.COV2.S, BNT162b2 and mRNA-1273, respectively. The absolute risk of CVST with thrombocytopenia within 28 days of first dose vaccination was 4.4 (95%CI 3.9-4.9), 0.7 (95%CI 0.2-2.4), 0.0 (95%CI 0.0-0.1) and 0.0 (95%CI 0.0-0.2) per million of first doses of ChAdOx1 nCov-19, Ad26.COV2.S, BNT162b2 and mRNA-1273, respectively. In recipients of ChAdOx1 nCov-19, the absolute risk of CVST, both with and without thrombocytopenia, was the highest in the 18-24 years age group (7.3 per million, 95%CI 2.8- 18.8 and 3.7 per million, 95%CI 1.0-13.3, respectively). The risk of CVST with thrombocytopenia in ChAdOx1 nCov-19 recipients was the lowest in the age group≥70 years (0.2, 95%CI 0.0-1.3). Age <60 compared to ≥60 was a predictor for CVST with thrombocytopenia (incidence rate ratio 5.79; 95%CI 2.98-11.24, p<0.001). The risk of CVST with thrombocytopenia within 28 days of first dose vaccination with ChAdOx1 nCov-19 was higher in younger age groups. The risk of CVST with thrombocytopenia was slightly increased in patients receiving Ad26.COV2.S, compared with the estimated background risk. The authors concluded that the risk of CVST with thrombocytopenia was not increased in recipients of SARS-CoV-2 mRNA vaccines.
Katarzyna Krzywicka, Anita van de Munckhof, Mayte Sánchez van Kammen, Mirjam R Heldner, Katarina Jood, Erik Lindgren, Turgut Tatlisumak, Jukka Putaala, Johanna A Kremer Hovinga, Saskia Middeldorp, Marcel M Levi, Charlotte Cordonnier, Marcel Arnold, Aeilko H Zwinderman, José M Ferro, Jonathan M Coutinho, Diana Aguiar de Sousa. Age-Stratified Risk of Cerebral Venous Sinus Thrombosis After SARS-CoV-2 Vaccination. Neurology Dec 2021, 10.1212/WNL.0000000000013148; DOI: 10.1212/WNL.0000000000013148.
The Impact of the COVID-19 Pandemic on Creutzfeldt-Jakob Disease Surveillance and Patient Care in the United Kingdom
Creutzfeldt-Jakob disease (CJD) is lethal and transmissible. In this article the authors assessed the impact of the COVID-19 pandemic on UK CJD surveillance. They hypothesised: i) disruptions prolonged diagnostic latency, ii) autopsy rates declined, and iii) COVID-19 infection negatively affected diagnosis, care and survival. They retrospectively investigated the first year of the pandemic, using the preceding year as a comparator, quantifying numbers of individuals assessed by the UK National CJD Research & Surveillance Unit (NCJDRSU) for suspected CJD, time-to-diagnosis, disease duration and autopsy rates. Furthermore, the impact of COVID-19 status on diagnosis, care and survival in CJD was evaluated. 148 individuals were diagnosed with CJD in the pandemic (from a total of 166 individuals assessed) compared to 141 in the comparator (from 145 assessed). No differences were identified in disease duration or time-to-diagnosis. Autopsy rates were unchanged. 20 individuals had COVID-19; 60% were symptomatic and 10% had severe disease. Disruptions to diagnosis and care were frequently identified. 40% of COVID-19 positive individuals died, however COVID-19 status did not significantly alter survival duration in CJD. The authors concluded that the COVID-19 pandemic has not impacted UK CJD case ascertainment or survival but diagnostic evaluation and clinical care of individuals have been affected.
Watson N, Kirby J, Kurudzhu H, Leitch M, MacKenzie J, Smith-Bathgate B, Smith C, Summers D, Green A, Pal S. The Impact of the COVID-19 Pandemic on Creutzfeldt-Jakob Disease Surveillance and Patient Care in the United Kingdom. Eur J Neurol. 2021 Dec 23. doi: 10.1111/ene.15228.
Association of the COVID-19 Outbreak with Acute Stroke Care in Switzerland
In Switzerland, the COVID-19 incidence during the first pandemic wave was high. In this article the authors aimed to assess the association of the outbreak with acute stroke care in Switzerland in spring 2020. This retrospective analysis has been based on the Swiss Stroke Registry, which includes consecutive patients with acute cerebrovascular events admitted to Swiss Stroke Units and Centers. The authors fitted a linear model to the weekly admission from 2018 and 2019 and used it to quantify deviations from the expected weekly admissions during from March, 13 to April 26, 2020 (the “lockdown period”). They compared characteristics and 3-month outcome of patients admitted during the lockdown period versus patients admitted during the same calendar period of 2018–2019.
28’310 patients admitted between 1 January 2018 and 26 April 2020 were included. Of these, 4’491 (15.9%) were admitted in the epochs March 13–April 26 of the years 2018 to 2020. During the lockdown in 2020, the weekly admissions dropped by up to 22% compared to rates expected from 2018 and 2019. During three consecutive weeks, weekly admissions fell below the 5% quantile (likelihood 0.38%). The proportion of intracerebral hemorrhage (ICH) among all registered admissions increased from 7.1% to 9.3% (P=0.006), and numerically less severe strokes were observed (median NIHSS from 3 to 2, P=0.07). The authors concluded that admissions and clinical severity of acute cerebrovascular events decreased substantially during the lockdown in Switzerland. Delivery and quality of acute stroke care were maintained.
De Marchis GM, Wright PR, Michel P, Strambo D, Carrera E, Dirren E, Luft AR, Wegener S, Cereda CW, Kägi G, Vehoff J, Gensicke H, Lyrer P, Nedeltchev K, Khales T, Bolognese M, Salmen S, Sturzenegger R, Bonvin C, Berger C, Schelosky L, Mono ML, Rodic B, von Reding A, Schwegler G, Tarnutzer AA, Medlin F, Humm AM, Peters N, Beyeler M, Kriemler L, Bervini D, Fandino J, Hemkens LG, Mordasini P, Arnold M, Fischer U, Bonati LH; Swiss Stroke Registry Investigators. Association of the COVID-19 Outbreak with Acute Stroke Care in Switzerland. Eur J Neurol. 2021 Dec 11. doi: 10.1111/ene.15209.
Multisystem Involvement in Post-acute Sequelae of COVID-19 (PASC)
The objective of this study was to describe cerebrovascular, neuropathic and autonomic features of post-acute sequelae of COVID-19 (PASC). This retrospective study evaluated consecutive patients with chronic fatigue, brain fog and orthostatic intolerance consistent with PASC. Controls included postural tachycardia syndrome patients (POTS) and healthy participants. Analyzed data included surveys and autonomic (Valsalva maneuver, deep breathing, sudomotor and tilt tests), cerebrovascular (cerebral blood flow velocity (CBFv) monitoring in middle cerebral artery), respiratory (capnography monitoring) and neuropathic (skin biopsies for assessment of small fiber neuropathy) testing and inflammatory/autoimmune markers. Nine PASC patients were evaluated 0.7±0.3 years after a mild COVID-19 infection, treated as home observations. Autonomic, pain, brain fog, fatigue and dyspnea surveys were abnormal in PASC and POTS (n=10), compared to controls (n=15). Tilt table test reproduced the majority of PASC symptoms. Orthostatic CBFv declined in PASC (-20.0±13.4%) and POTS (-20.3±15.1%), compared to controls (-3.0±7.5%,p=0.001) and was independent of end-tidal carbon dioxide in PASC, but caused by hyperventilation in POTS. Reduced orthostatic CBFv in PASC included both subjects without (n=6) and with (n=3) orthostatic tachycardia. Dysautonomia was frequent (100% in both PASC and POTS) but was milder in PASC (p=0.013). PASC and POTS cohorts diverged in frequency of small fiber neuropathy (89% vs. 60%) but not in inflammatory markers (67% vs. 70%). Supine and orthostatic hypocapnia was observed in PASC. The authors concluded that PASC following mild COVID-19 infection is associated with multisystem involvement including: 1) cerebrovascular dysregulation with persistent cerebral arteriolar vasoconstriction; 2) small fiber neuropathy and related dysautonomia; 3) respiratory dysregulation; 4) chronic inflammation.
Novak P, Mukerji SS, Alabsi HS, Systrom D, Marciano SP, Felsenstein D, Mullally WJ, Pilgrim DM. Multisystem Involvement in Post-acute Sequelae of COVID-19 (PASC). Ann Neurol. 2021 Dec 24. doi: 10.1002/ana.26286.
A longitudinal seizure outcome following the COVID-19 pandemic in 2020 and 2021: Transient exacerbation or sustainable mitigation
The objective of this article was to study the longitudinal seizure outcomes of people with epilepsy (PWE) following the acute and chronic phases of the coronavirus disease 2019 (COVID-19) pandemic.
Consecutive PWE who were treated at the epilepsy center of Hiroshima University Hospital between 2018 and 2021 were enrolled. The authors evaluated the incidence of seizure frequency increase or decrease following the pandemic during observational periods in 2020 and 2021. Data between 2018 and 2019 were used as a control set. The sustainability of the altered seizure frequency condition was evaluated throughout the study period. They analyzed the clinical, psychological, and social factors associated with PWE with seizure exacerbation or amelioration. Among the 223 PWE who were evaluated (mean age 37.8 ± 16.3 years), seizure frequency increased for 40 (16.8%) and decreased for 34 (15.2%) after the pandemic began. While seizure exacerbation tended to be a transient episode during 2020, seizure amelioration was likely to maintain excellent status over the observation periods; the sustainability of the altered seizure frequency condition was more prominent for amelioration than exacerbation (p < 0.001). Seizure exacerbation was significantly associated with “no housemate” (odds ratio [OR] 3.37; p = 0.045) and “comorbidity of insomnia” (OR 5.80; p = 0.004). Conversely, “structural abnormality of MRI” (OR 2.57; p = 0.039) and “two-generation householding” (OR 3.70; p = 0.004) were independently associated with seizure amelioration. The authors concluded that this longitudinal observation confirmed that seizure exacerbation and amelioration emerged during the COVID-19 pandemic. The COVID-19 pandemic has shed light on the stark difference that social support systems can make on outcomes for PWE.
Neshige S, Aoki S, Takebayashi Y, Shishido T, Yamazaki Y, Iida K, Maruyama H. A longitudinal seizure outcome following the COVID-19 pandemic in 2020 and 2021: Transient exacerbation or sustainable mitigation. J Neurol Sci. 2021 Dec 17;434:120100. doi: 10.1016/j.jns.2021.120100.
APOE ε4 associates with increased risk of severe COVID-19, cerebral microhaemorrhages and post-COVID mental fatigue: a Finnish biobank, autopsy and clinical study
Apolipoprotein E ε4 allele (APOE4) has been shown to associate with increased susceptibility to SARS-CoV-2 infection and COVID-19 mortality in some previous genetic studies, but information on the role of APOE4 on the underlying pathology and parallel clinical manifestations is scarce. In this article the authors studied the genetic association between APOE and COVID-19 in Finnish biobank, autopsy and prospective clinical cohort datasets. In line with previous work, their data on 2611 cases showed that APOE4 carriership associates with severe COVID-19 in intensive care patients compared with non-infected population controls after matching for age, sex and cardiovascular disease status. Histopathological examination of brain autopsy material of 21 COVID-19 cases provided evidence that perivascular microhaemorrhages are more prevalent in APOE4 carriers. Finally, they analysis of post-COVID fatigue in a prospective clinical cohort of 156 subjects revealed that APOE4 carriership independently associates with higher mental fatigue compared to non-carriers at six months after initial illness. The authors concluded that the present data on Finns suggests that APOE4 is a risk factor for severe COVID-19 and post-COVID mental fatigue and provides the first indication that some of this effect could be mediated via increased cerebrovascular damage. Further studies in larger cohorts and animal models are warranted.
Kurki SN, Kantonen J, Kaivola K, Hokkanen L, Mäyränpää MI, Puttonen H; FinnGen, Martola J, Pöyhönen M, Kero M, Tuimala J, Carpén O, Kantele A, Vapalahti O, Tiainen M, Tienari PJ, Kaila K, Hästbacka J, Myllykangas L. APOE ε4 associates with increased risk of severe COVID-19, cerebral microhaemorrhages and post-COVID mental fatigue: a Finnish biobank, autopsy and clinical study. Acta Neuropathol Commun. 2021 Dec 23;9(1):199. doi: 10.1186/s40478-021-01302-7.
Characteristics and Risk Factors of Persistent Neuropathic Pain in Recovered COVID-19 Patients
The objective of this case-control study was to assess risk factors for persistent neuropathic pain in subjects recovered from COVID-19 and to study the serum level of neurofilament light chain (NFL) in those patients. 45 patients with post COVID-19 pain and another 45 age and sex-matched healthcare workers who recovered from COVID-19 without pain were included. Participants were subjected to medical history taking, screening for depressive disorders, comprehensive neurological examination, and pain evaluation using the Douleur Neuropathique en 4 questions (DN4). All patients who had a score at least 4/10 on DN4 were included. The serum NFL level was measured for both groups at the time of patients’ enrolment. The frequency of depression, moderate and severe COVID-19 cases, disease duration and serum ferritin were significantly higher in the cases with post COVID-19 pain than controls. Binary logistic regression revealed that depression, azithromycin use, moderate and severe COVID-19 increased the odds of post COVID-19 pain by 4.462, 5.444, 4.901, & 6.276 times, respectively. Cases with post COVID-19 pain had significantly higher NFL (11.34 ± 9.7, 95%CI: 8.42 – 14.25) than control group (7.64 ± 5.40, 95%CI: 6.02-9.27), (P-value= 0.029). Patients with allodynia had significantly higher NFL (14.96 ± 12.41, 95%CI: 8.58-21.35) compared to those without (9.14 ± 6.99, 95%CI: 6.43-11.85) (P-value= 0.05). The authors concluded that depression, azithromycin, moderate and severe COVID-19 are independent predictors of persistent post COVID-19 pain. Serum NFL may serve as a potential biomarker for persistent neuropathic pain after COVID-19.
Magdy R, Eid RA, Fathy W, Abdel-Aziz MM, Ibrahim RI, Yehia A, Sheemy MS, Hussein M. Characteristics and Risk Factors of Persistent Neuropathic Pain in Recovered COVID-19 Patients. Pain Med. 2021 Dec 21:pnab341. doi: 10.1093/pm/pnab341.
Barriers to telemedicine among physicians in epilepsy care during the COVID-19 pandemic: A national-level cross-sectional survey in Japan
This study aimed to investigate the factors affecting the unwillingness of physicians involved in epilepsy care to continue telemedicine during the coronavirus disease 2019 (COVID-19) pandemic in Japan. This was a national-level cross-sectional survey initiated by Japan Young Epilepsy Section (YES-Japan) which is a national chapter of The Young Epilepsy Section of the International League Against Epilepsy (ILAE-YES). The authors asked physicians who conducted telemedicine in patients with epilepsy (PWE) during the COVID-19 pandemic at four clinics and 21 hospitals specializing in epilepsy care in Japan from March 1 to April 30, 2021. The following data were collected: (1) participant profile, (2) characteristics of PWE treated by telemedicine, and (3) contents and environmental factors of telemedicine. Statistically significant variables (p < 0.05) in the univariate analysis were analyzed in a multivariate binary logistic regression model to detect the independently associated factors with the unwillingness to continue telemedicine. Among the 115 respondents (response rate: 64%), 89 were included in the final analysis. Of them, 60 (67.4%) were willing to continue telemedicine, and 29 (32.6%) were unwilling. In the univariate binary logistic regression analysis, age (Odds ratio [OR] = 1.84, 95% confidence interval [CI] 1.10-3.09, p = 0.02), psychiatrist (OR = 5.88, 95% CI 2.15-16.08, p = 0.001), hospital (OR = 0.10, 95% CI 0.01-0.94, p = 0.04), the number of COVID-19 risk factors in the participant (OR = 2.88, 95% CI 1.46-5.69, p = 0.002), the number of COVID-19 risk factors in the cohabitants (OR = 2.52, 95% CI 1.05-6.01, p = 0.04), COVID-19 epidemic area (OR = 4.37, 95% CI 1.18-16.20, p = 0.03), consultation time during telemedicine (OR = 2.51, 95% CI 1.32-4.76, p = 0.005), workload due to telemedicine (OR = 4.17, 95% CI 2.11-8.24, p < 0.001) were statistically significant. In the multivariate binary logistic regression analysis, workload due to telemedicine (OR = 4.93, 95% CI 1.96-12.35) was independently associated with the unwillingness to continue telemedicine. The authors concluded that this national-level cross-sectional survey found that workload due to telemedicine among physicians involved in epilepsy care was independently associated with the unwillingness to continue telemedicine.
Kubota T, Kuroda N, Horinouchi T, Ikegaya N, Kitazawa Y, Kodama S, Kuramochi I, Matsubara T, Nagino N, Neshige S, Soga T, Takayama Y, Sone D. Barriers to telemedicine among physicians in epilepsy care during the COVID-19 pandemic: A national-level cross-sectional survey in Japan. Epilepsy Behav. 2021 Dec 3;126:108487. doi: 10.1016/j.yebeh.2021.108487.
Persistent white matter changes in recovered COVID-19 patients at the 1-year follow-up
There is growing evidence that severe acute respiratory syndrome coronavirus 2 can affect the CNS. However, data on white matter and cognitive sequelae at the one-year follow-up are lacking. In this article the authors explored these characteristics and investigated 22 recovered coronavirus disease 2019 (COVID-19) patients and 21 matched healthy controls. Diffusion tensor imaging, diffusion kurtosis imaging and neurite orientation dispersion and density imaging were performed to identify white matter changes, and the subscales of the Wechsler Intelligence scale were used to assess cognitive function. Correlations between diffusion metrics, cognitive function, and other clinical characteristics were then examined. They also conducted subgroup analysis based on patient admission to the intensive care unit. The corona radiata, corpus callosum and superior longitudinal fasciculus had lower volume fraction of intracellular water in the recovered COVID-19 group than in the healthy control group. Patients who had been admitted to the intensive care unit had lower fractional anisotropy in the body of the corpus callosum than those who had not. Compared with the healthy controls, the recovered COVID-19 patients demonstrated no significant decline in cognitive function. White matter tended to present with fewer abnormalities for shorter hospital stays and longer follow-up times. Lower axonal density was detected in clinically recovered COVID-19 patients after one year. Patients who had been admitted to the intensive care unit had slightly more white matter abnormalities. No significant decline in cognitive function was found in recovered COVID-19 patients. The authors concluded underlying that the duration of hospital stay may be a predictor for white matter changes at the one-year follow-up.
Huang S, Zhou Z, Yang D, Zhao W, Zeng M, Xie X, Du Y, Jiang Y, Zhou X, Yang W, Guo H, Sun H, Liu P, Liu J, Luo H, Liu J. Persistent white matter changes in recovered COVID-19 patients at the 1-year follow-up. Brain. 2021 Dec 16:awab435. doi: 10.1093/brain/awab435.
CD19 B cell repopulation after ocrelizumab, alemtuzumab and cladribine: Implications for SARS-CoV-2 vaccinations in multiple sclerosis
Ocrelizumab maintains B-cell depletion via six-monthly dosing. Whilst this controls relapsing multiple sclerosis, it also inhibits seroconversion following SARS-CoV-2 vaccination unlike that seen following alemtuzumab and cladribine treatment. Emerging reports suggest that 1-3% B-cell repopulation facilitates seroconversion after CD20-depletion. The objective of this study was to determine the frequency of B-cell repopulation levels during and after ocrelizumab treatment. Relapse data, lymphocyte and CD19 B-cell numbers were obtained following requests to clinical trial data-repositories. Information was extracted from the phase II ocrelizumab extension (NCT00676715) trial and the phase III cladribine tablet (NCT00213135) and alemtuzumab (NCT00530348/NCT00548405) trials obtained clinical trial data requests.
Only 3-5% of people with MS exhibit 1% B-cells at 6 months after the last infusion following 3-4 cycles of ocrelizumab, compared to 50-55% at 9 months, and 85-90% at 12 months. During this time relapses occurred at consistent disease-breakthrough rates compared to people during standard therapy. In contrast most people (90-100%) exhibited more than 1% B-cells during treatment with either cladribine or alemtuzumab. The authors concluded that most people demonstrate B cell repletion within 3 months of the last treatment of alemtuzumab and cladribine. However, few people repopulate peripheral B-cells with standard ocrelizumab dosing. Controlled studies are warranted to examine a view that delaying the dosing interval by 3-6 months may allow more people to potentially seroconvert after vaccination.
Baker D, MacDougall A, Kang AS, Schmierer K, Giovannoni G, Dobson R. CD19 B cell repopulation after ocrelizumab, alemtuzumab and cladribine: Implications for SARS-CoV-2 vaccinations in multiple sclerosis. Mult Scler Relat Disord. 2021 Dec 4;57:103448. doi: 10.1016/j.msard.2021.103448.
Neurologic and cognitive sequelae after SARS-CoV2 infection: Different impairment for ICU patients
The exact incidence of neurological and cognitive sequelae of COVID-19 in the long term is yet unknown. The aim of this research is to investigate the type of neurological and cognitive impairment in COVID-19 cases of different severity. Two hundred fifteen patients, who had developed COVID-19, were examined 4 months after the diagnosis by means of neurological exam and extensive cognitive evaluation, investigating general cognition, memory, verbal fluency, visuospatial abilities and executive functions. Fifty-two of them were treated in intensive care unit (ICU patients), whereas 163 were not hospitalized (non-ICU patients). Neurological deficits were found in 2/163 (1.2%) of non-ICU and in 7/52 (13.5%) of the ICU cases, all involving the peripheral nervous system. ICU patients performed significantly worse in all the neuropsychological tests and showed a worse age- and education-corrected cognitive impairment: Cognitive Impairment Index (CII) was higher in ICU than in non-ICU patients (median ICU 3 vs 2, p = .001). CII significantly correlated with age in both groups, was unrelated to length of follow- up, diabetes and hypertension and – only for ICU patients- to PaO2/FiO2 at ICU admission. The authors concluded that the obtained results support the greater susceptibility of COVID-19 patients, treated in ICU, to develop neurological deficits and cognitive impairment at a four-month follow up, as compared to cases with mild/moderate symptoms.
Mattioli F, Piva S, Stampatori C, Righetti F, Mega I, Peli E, Sala E, Tomasi C, Indelicato AM, Latronico N, De Palma G. Neurologic and cognitive sequelae after SARS-CoV2 infection: Different impairment for ICU patients. J Neurol Sci. 2021 Nov 26;432:120061. doi: 10.1016/j.jns.2021.120061.
Epilepsy is overrepresented among young people who died from COVID-19: Analysis of nationwide mortality data in Hungary
Studies examining epilepsy as a COVID-related death risk have come to conflicting conclusions. The aim of this study was to assess the prevalence of epilepsy among COVID-related deaths in Hungary.
Each COVID-19 infection case is required to be reported on a daily basis to the National Public Health Center of Hungary. This online report includes the beginning and end of the infection, as well as information on comorbidities. Death during infection is regarded as COVID-related. The anonymized data of each deceased patient are published on an information website (www.koronavirus.gov.hu) and provides up-to-date information on each patient with the date of death, the patient’s sex, age, and chronic illness. There were 11,968 patients who died of COVID-19 in Hungary between 13 March 2020 and 23 January 2021. Among 11,686 patients with no missing values for comorbidities, 255 patients had epilepsy (2.2%). Epilepsy was much more common among those who died at a young age: 9.3% of those who died under the age of 50 had epilepsy, compared with only 1.3% in those over the age of 80. The younger an age group was, the higher was the prevalence of epilepsy. The authors concluded that patients who died of COVID-19 under the age of 50 were 10 to 20 times more likely to have epilepsy than what would have been expected from epidemiological data highlighting the need for increased protection of young people with epilepsy from COVID-19 infection and the development of a vaccination strategy accordingly.
Horváth RA, Sütő Z, Cséke B, Schranz D, Darnai G, Kovács N, Janszky I, Janszky J. Epilepsy is overrepresented among young people who died from COVID-19: Analysis of nationwide mortality data in Hungary. Seizure. 2021 Dec 1;94:136-141. doi: 10.1016/j.seizure.2021.11.013.