I would like to report on the 6 months that I spent at the centre of dizziness and balance disorders in the Neurology Department (Head: Professor Dr. Thomas Münte) at the University Hospital of Schleswig Holstein in Lübeck, Germany, as a fellow in the Educational Fellowship Programme of the European Federation of Neurological Societies (EFNS). Professor Christoph Helmchen, the head of the centre of dizziness and balance disorders in Lübeck, was my tutor during this period and I had the chance to join his research group.
 I participated in the everyday work at this special dizziness centre and through this activity I got familiar with the clinical approach (special history taking, neuro-otological and clinical neuro-ophthalmologic examinations) that is required for a precise diagnosis. Among all I gained routine in applying the different reposition maneuvers in different cases of benign paroxysmal positional vertigo (BBPV). Besides these clinical benefits, I could additionally get an
I participated in the everyday work at this special dizziness centre and through this activity I got familiar with the clinical approach (special history taking, neuro-otological and clinical neuro-ophthalmologic examinations) that is required for a precise diagnosis. Among all I gained routine in applying the different reposition maneuvers in different cases of benign paroxysmal positional vertigo (BBPV). Besides these clinical benefits, I could additionally get an  impression of the German heath care system as well. I got to know various diagnostic tests in the laboratory and I gained practice both in performing these tests and in evaluating the results. We collected normal data for the ocular vestibular evoked myogenic potentials (o-VEMP) in the Laboratory. The members of the dizziness centre, both doctors, and the assistants in the laboratory were very helpful. Furthermore I had the chance to participate in a
impression of the German heath care system as well. I got to know various diagnostic tests in the laboratory and I gained practice both in performing these tests and in evaluating the results. We collected normal data for the ocular vestibular evoked myogenic potentials (o-VEMP) in the Laboratory. The members of the dizziness centre, both doctors, and the assistants in the laboratory were very helpful. Furthermore I had the chance to participate in a  one day long regional training for dizziness, which was organised at the end of May by the colleagues of the dizziness centre in Bad Segeberg.
one day long regional training for dizziness, which was organised at the end of May by the colleagues of the dizziness centre in Bad Segeberg.
Besides collecting clinical experience, I participated in research projects as well. With the help of the research team members (Professor Helmchen, Andreas Sprenger and Björn Machner) I started two observational studies.
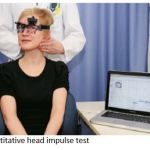
One research project aimed to evaluate the influence of history on the reliability of the clinical head impulse test (cHIT). This clinical test helps to assess the vestibular function (vestibulo-ocular reflex) by testing gaze stability during rapid head motion. The clinical evaluation was done both before and after the clinical history was taken, to see how much influence the history has on the evaluation of the clinical investigator. Afterwards the clinical ratings were compared to quantitative measurements done by video-HIT (qHIT). It remains open at present whether the combination of both (cHIT and qHIT) is supportive (increasing sensitivity) or confusing (decreasing sensitivity) in the final, clinical evaluation.
The other project aims to identify the effects of Labyrinth Anesthesia in Meniere’s disease. During the procedure the patients receive a Lidocaine injection into the middle ear. The procedure is clinically effective in inducing a long attack free period, but the mode of action is unknown. Therefore we examine the electrophysiological changes of the vestibulo-cochlear system and the inner ear changes using contrast enhanced MRI. We performed several pilot imaging studies to identify the most suitable recording parameters. I will continue the study in cooperation with the members of the research team.
I must especially thank Professor Christoph Helmchen and Andreas Sprenger for their support during my stay. Furthermore I would like to thank the EFNS for giving me the opportunity and the financial support for this clinical and research activity through the Scholarship Programme.














