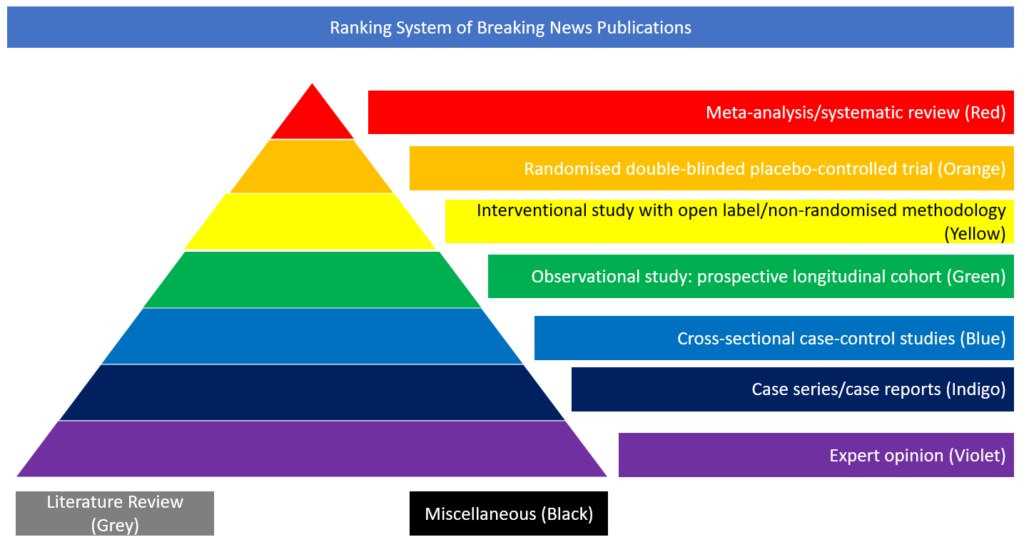
Literature Review
Anosmia, stroke, paralysis, cranial nerve deficits, encephalopathy, delirium, meningitis, and seizures are some of the neurological complications in patients with COVID-19.
There remains a challenge to determine the extent to which neurological abnormalities in COVID-19 are caused by SARS-Cov2 itself, the exaggerated cytokine response it triggers, and/or the resulting hypercoagulopathy. In this article, the authors review reports that address neurological manifestations in patients with COVID-19 presenting with acute neurological symptoms, such as stroke. They discuss the different neurobiological processes and mechanisms that may underlie the links between COVID-19 and damage to the brain, cranial nerves, peripheral nerves, and muscles. Finally, they propose a basic “NeuroCovid” classification scheme that integrates these concepts, highlight some of the short-term challenges for the practice of neurology today and consider possible longer-term sequalae of COVID-19, such as depression, obsessive-compulsive disorder, insomnia, cognitive decline, accelerated ageing, Parkinson’s disease, or Alzheimer’s disease that might emerge in the future.
https://content.iospress.com/articles/journal-of-alzheimers-disease/jad200581