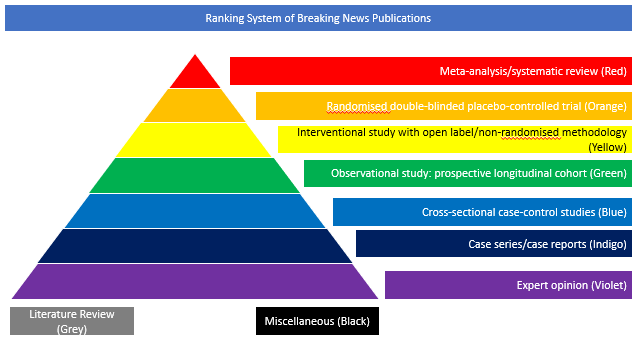
Cross-sectional case-control studies (Blue)
During the COVID-19 outbreak, the presence of extensive white matter microhaemorrhages was detected by brain MRIs. The goal of this study was to investigate the origin of this atypical hemorrhagic complication. Between March 17 and May 18, 2020, 80 patients with severe COVID-19 infections were admitted for acute respiratory distress syndrome to intensive care units at the University Hospitals of Strasbourg for whom a brain MRI for neurological manifestations was performed. 19 patients (24%) with diffuse microhaemorrhages were compared to 18 control patients with COVID-19 and normal brain MRI. The first hypothesis was hypoxaemia. The latter seemed very likely since respiratory failure was longer and more pronounced in patients with microhaemorrhages (prolonged endotracheal intubation (p = 0.0002), higher FiO2 (p = 0.03), increased use of extracorporeal membrane oxygenation (p = 0.04)). Another relevant hypothesis, the role of microangiopathy, was also considered, since patients with microhaemorrhages presented with a higher increase in D-dimers (p = 0.01) and a (non-significant) tendency to more frequent thrombotic events (p = 0.12).
Another hypothesis tested was the role of kidney failure, which was more severe in the group with diffuse microhaemorrhages (higher creatinine level [median of 293 µmol/L versus 112 µmol/L, p = 0.04] and more dialysis was performed in this group during the ICU stay [12 versus 5 patients, p = 0.04]). The authors concluded that blood–brain barrier dysfunction secondary to hypoxaemia and high concentration of uraemic toxins seem to be the main mechanisms leading to critical illness-associated cerebral microbleeds, and this complication remains to be frequently described in severe COVID-19 patients.
DOI: https://doi.org/10.1007/s00415-020-10313-8